Celiac disease is not simply a digestive sensitivity or a dietary preference—it is a lifelong autoimmune condition that affects how the body processes nutrients and maintains immune balance. In people with celiac disease, eating gluten sets off an immune reaction that damages the small intestine, even when symptoms seem mild or unrelated to digestion. Over time, this damage can affect multiple organ systems, making early recognition and structured care essential.
Many patients who seek evaluation for unexplained anemia, fatigue, or bone weakness eventually discover the underlying cause through specialized gastroenterology care at Liv Hospital, where intestinal and immune-related conditions are assessed together rather than in isolation.
How the Immune System Drives Celiac Disease
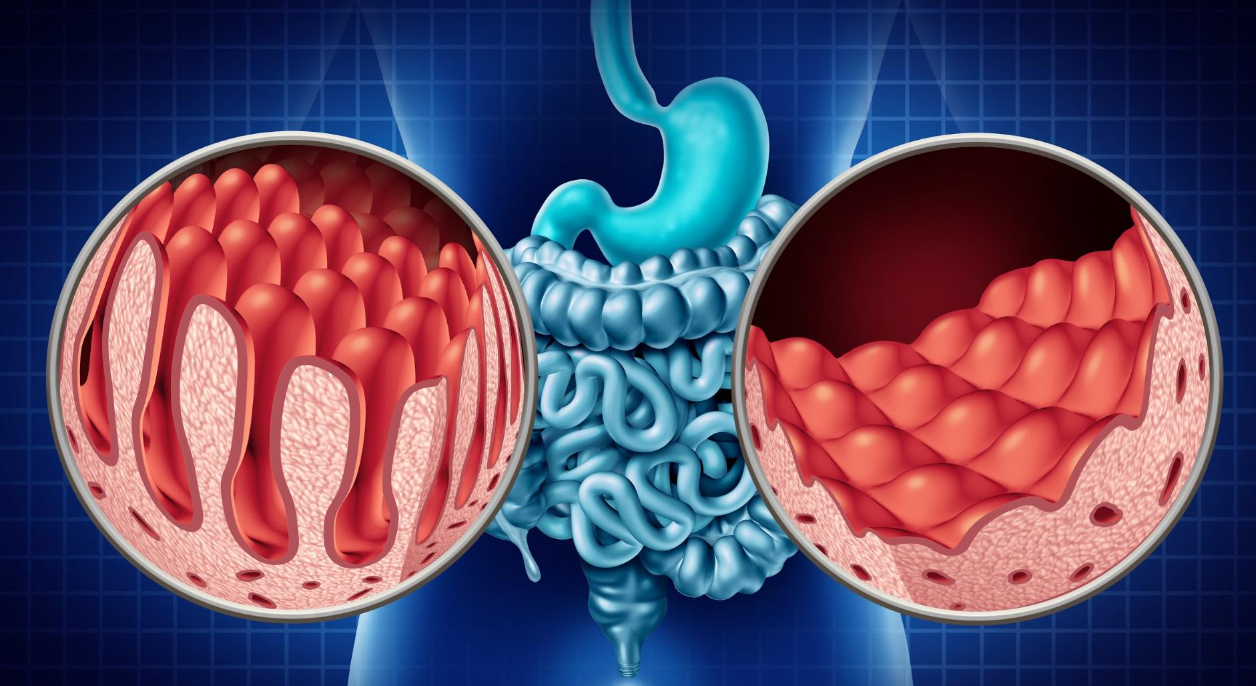
Celiac disease develops in genetically predisposed individuals when gluten proteins trigger an abnormal immune response. Instead of tolerating gluten as a harmless dietary component, the immune system attacks the lining of the small intestine. This reaction flattens the intestinal villi—tiny finger-like projections responsible for absorbing nutrients.
As the villi become damaged, the body struggles to absorb iron, calcium, vitamins, and other essential nutrients. This explains why celiac disease often presents with symptoms that extend far beyond the digestive tract, even before significant stomach or bowel complaints appear.
Why Celiac Disease Often Goes Undetected
One of the most challenging aspects of celiac disease is its unpredictable presentation. Some individuals experience classic digestive symptoms, while others develop silent or atypical forms that delay diagnosis for years.
Common non-digestive signs include:
- Persistent fatigue or brain fog
- Iron-deficiency anemia resistant to supplements
- Bone pain or early osteoporosis
- Recurrent mouth ulcers
- Skin conditions such as dermatitis herpetiformis
Because these symptoms overlap with many other conditions, celiac disease is frequently overlooked unless testing is performed while gluten is still part of the diet.
Celiac Disease Is Not a Food Allergy or Intolerance
It is important to distinguish celiac disease from wheat allergy and non-celiac gluten sensitivity. A wheat allergy causes immediate allergic reactions, while gluten sensitivity may lead to discomfort without intestinal damage. Celiac disease, however, involves an autoimmune attack that causes measurable injury to the intestine, even when symptoms are subtle.
This distinction matters because untreated celiac disease can lead to serious long-term complications, regardless of symptom severity.
How Diagnosis Is Confirmed
Diagnosis begins with blood tests that detect antibodies produced during the immune response to gluten. If these markers are positive, an upper endoscopy with small bowel biopsy is typically performed to confirm intestinal damage.
This diagnostic pathway is central to GASTROENTEROLOGY Celiac Disease management, as accurate diagnosis ensures that patients are not placed on unnecessary dietary restrictions without medical confirmation.
Long-Term Health Risks of Untreated Celiac Disease
When celiac disease remains undiagnosed or unmanaged, chronic inflammation and malabsorption can affect nearly every system in the body. Potential complications include:
- Osteoporosis and increased fracture risk
- Infertility or recurrent pregnancy loss
- Growth delays in children
- Neurological symptoms such as numbness or balance issues
- Increased risk of certain intestinal cancers
These risks exist even in patients who feel “mostly fine,” reinforcing why strict adherence to treatment is critical.
Treatment Is Simple in Concept, Complex in Practice
The only effective treatment for celiac disease is a lifelong, strict gluten-free diet. While this sounds straightforward, gluten can hide in processed foods, medications, and even supplements. Even small exposures can reactivate immune damage without obvious symptoms.
Successful management often requires ongoing medical follow-up, nutritional guidance, and periodic monitoring to ensure intestinal healing and nutrient recovery.
Living Well After a Celiac Diagnosis
With proper diagnosis and consistent dietary management, most patients experience intestinal healing and symptom improvement. Energy levels rise, nutrient deficiencies correct, and long-term risks decline significantly. Beyond medical treatment, many people find that learning how to balance nutrition, stress, and daily habits helps them adapt more confidently to life with celiac disease. Lifestyle-focused platforms like live and feel are often explored as supportive resources for maintaining overall well-being alongside medical care.